The good and bad European health trends explained
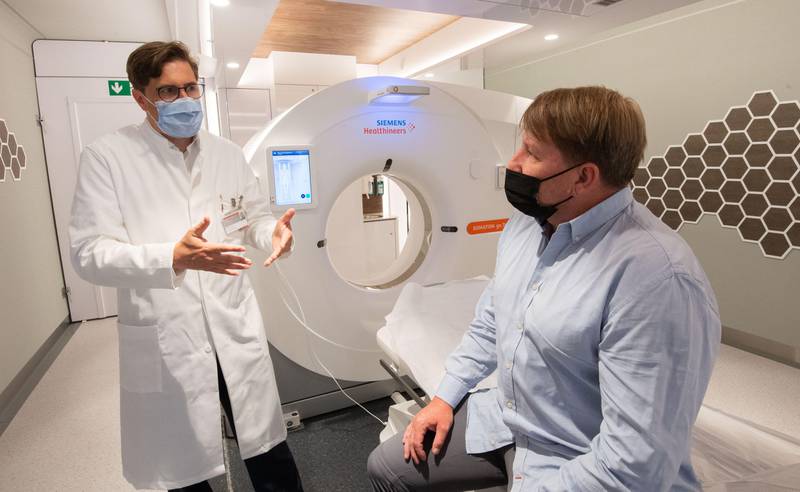
The World Health Organisation has urged Europe to put health at the heart of its socioeconomic recovery from the coronavirus pandemic. Its European Health Report 2021, published on Thursday, describes the challenge as daunting but suggests there is a "critical window" in which meaningful action can be taken.
The report identifies several successes and failures in Europe's health outlook, with a reduction in cardiovascular disease countered by a general worsening of mental health. “We have a stark choice at this juncture almost two years into the pandemic,” said Dr Hans Henri P Kluge, WHO regional director for Europe.
“We can prioritise the health sector as never before, with an urgent focus on long-neglected issues including mental health, recognising health systems and health workers as essential pillars of socioeconomic recovery and key to preparing for future shocks."
A WHO representative told The National the body was monitoring the crisis but does not think it will distract European countries from addressing existing health inequalities.
As well as setting out a framework for action, the triannual report monitors health indicators such as universal health coverage, non-communicable diseases and environmental health.
In concert with report co-author Dr Ausra Zelviene, WHO consultant and head of psychoactive substance use, prevention and co-ordination division at the drug, tobacco, and alcohol control department with the government of Lithuania, The National highlights some of Europe's health successes and failures.
Between 2010 and 2018, premature mortality because of cardiovascular diseases fell by almost 20 per cent.
The trend is not a new one, with deaths related to the heart decreasing now for 25 years.
Dr Zelviene identifies two factors in this reduction: better health behaviour and improved healthcare which now acts as an early warning system for problems.
"Primary healthcare [now] sees the intermediate risk factors like race blood compression, race blood glucose, race blood lipids, and obesity … and reacts to these conditions," she said.
Going deeper into the data, four out of five incidences of cardiovascular disease are either heart attacks or strokes, and one third is experienced by those under 70.
The risk of cardiovascular disease is also much higher in women than in men.
"There is a greater prevalence of behavioural risk factors in men like unhealthy diets, physical inactivity, tobacco smoking," Dr Zelviene said.
Cancer deaths decrease by 10 per cent
The picture with cancers is less clear cut than cardiovascular as cancer still accounts for more than 20 per cent of all deaths, a situation exacerbated by the pandemic’s impact on screening and treatment.
Yet decreasing deaths have to be categorised as a success, and further lifestyle interventions and narrowing in health disparities could ease the trajectory.
"Around one third of deaths from cancer are due to tobacco use and other unhealthy behaviours like high alcohol and low fruit and vegetable consumption," Dr Zelviene said.
"One of the main messages would be that many cancers can be cured if detected early and treated effectively."
This is where health inequities need urgent redress.
"Many health systems in low and middle income countries are not very well prepared to manage this burden and large numbers of cancer patients do not have access to timely and quality diagnosis and treatment," Dr Zelviene said.
"Comprehensive treatment is available in more than 90 per cent of high income countries and less than 15 per cent of low income countries.
Lower maternal, newborn and child mortality
All countries in the WHO European region have met the WHO target for maternal mortality of fewer than 70 per 100,000 live births by 2030. The region’s average rate is at 13 per 100,000 live births, as of 2017.
Almost all countries in the WHO European region have met the target for newborn and child mortality rate of fewer than 12 and 25 deaths per 1,000 live births, respectively.
Dr Zelviene said the main factor in this propitious trend is improved access to, and provision of, care to poor people.
"Women who are in trouble, that is both before pregnancy and during pregnancy, they will get appropriate care and if something bad happens those events will be investigated, and the knowledge is transmitted further in order to avoid them in future," she said.
"One more [very important factor] is the continuous education both of healthcare providers and patients to see the earliest signs of medical complications of pregnancy."
Europe's health failures
More smokers than global average
Twenty-six per cent of the adult population still smoke tobacco compared to the global average of 23.6 per cent.
This is not the full picture, however, as Europe started from a very high level - 35 per cent at the millennium.
Interestingly, while the prevalence of male smokers has dropped during this period, the prevalence of female smokers has plateaued at about 18 per cent.
A reason for the slowness of the decline is regulatory.
"Only 14 out of all 53 countries in the region prohibit smoking in all out of places and public places," Dr Zelviene said.
She also highlighted the fierce opposition of the tobacco industry as an impediment to robust regulatory change, and many countries in Europe fail to tax big tobacco proportionately.