Medicaid-eligible people who aren’t enrolled far more likely to delay care
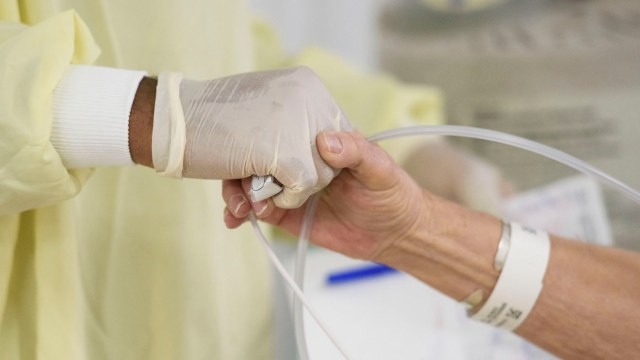
Adults who are eligible for Medicaid but not enrolled in the program are more likely to delay care due to costs, according to an analysis published Tuesday by the Urban Institute.
The survey found 21.4 percent of non-Medicaid enrolled individuals delay medical care due to the cost, compared to only 7.3 percent of enrollees and 9.5 percent of Medicaid-eligible individuals with private insurance.
Eligible but unenrolled adults were less likely than Medicaid enrollees to have visited a doctor in the last year, 23.4 percent compared to 65.4 percent. UnenrolledRead More : Sophisticated veterinary medicine in the HV adults were also less likely to have a prescription filled, 27.8 percent to 67 percent, and less likely to have stayed in a hospital, 2.5 percent versus 12.6 percent. Around 37 percent of Medicaid-eligible adults who are not enrolled reported having a usual source of care, compared to 69.9 percent of Medicaid enrollees and 66.8 percent of Medicaid-eligible individuals with private insurance.
The analysis found uninsured Medicaid-eligible adults also spent more on out-of-pocket health expenses.
“Researchers conclude that being eligible for Medicaid does not equate to being covered by Medicaid or private insurance, as some have suggested,” a brief on the analysis wrote. “People enrolled in health insurance face fewer obstacles and better outcomes.”
The analysis comes as millions of people were recently pushed off state Medicaid rolls amid the end of pandemic-era policies.
Data shows nearly 5.5 million people were purged from state Medicaid rolls across 45 states and the District of Columbia, according to health policy research group KFF.
Most individuals were removed for “procedural” reasons, including missing or incorrect paperwork, or outdated contact information, though they may still be eligible.
Last year, Congress gave the Centers for Medicare and Medicaid Services more power to ensure states are not improperly removing Medicaid beneficiaries. The agency is allowed to instruct states to pause procedural terminations, file a corrective action plan or stop federal funding.
In the wake of the millions purged, the Biden administration has faced growing pressure to guarantee people are protected.
The analysis used data from the Medical Expenditure Panel Survey Household Component.
The survey found 21.4 percent of non-Medicaid enrolled individuals delay medical care due to the cost, compared to only 7.3 percent of enrollees and 9.5 percent of Medicaid-eligible individuals with private insurance.
Eligible but unenrolled adults were less likely than Medicaid enrollees to have visited a doctor in the last year, 23.4 percent compared to 65.4 percent. Unenrolled
The analysis found uninsured Medicaid-eligible adults also spent more on out-of-pocket health expenses.
“Researchers conclude that being eligible for Medicaid does not equate to being covered by Medicaid or private insurance, as some have suggested,” a brief on the analysis wrote. “People enrolled in health insurance face fewer obstacles and better outcomes.”
The analysis comes as millions of people were recently pushed off state Medicaid rolls amid the end of pandemic-era policies.
Data shows nearly 5.5 million people were purged from state Medicaid rolls across 45 states and the District of Columbia, according to health policy research group KFF.
Most individuals were removed for “procedural” reasons, including missing or incorrect paperwork, or outdated contact information, though they may still be eligible.
Last year, Congress gave the Centers for Medicare and Medicaid Services more power to ensure states are not improperly removing Medicaid beneficiaries. The agency is allowed to instruct states to pause procedural terminations, file a corrective action plan or stop federal funding.
In the wake of the millions purged, the Biden administration has faced growing pressure to guarantee people are protected.
The analysis used data from the Medical Expenditure Panel Survey Household Component.
Source: thehill.com