Health specialists clash over use of certain drugs
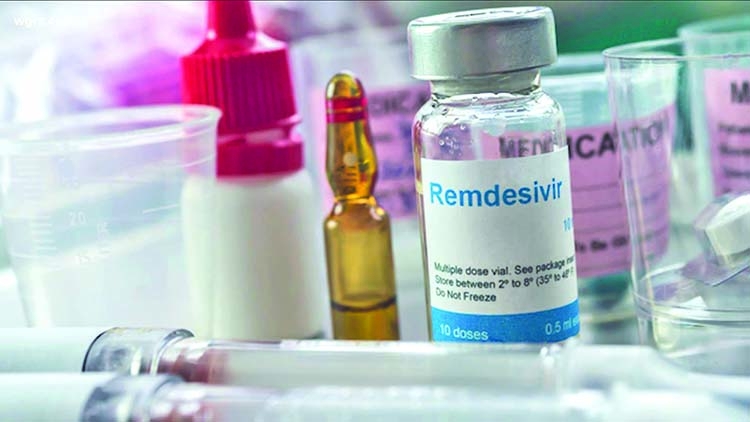
Health officials all over the world are actually clashing over the use of certain prescription drugs for COVID-19, leading to different treatment options for patients based on their current address. On Friday, a World Health Organization suggestions panel advised against using the antiviral remdesivir for hospitalized clients, saying there's no evidence it improves survival or avoids the necessity for breathing machines. But in the US and many other countries, the medication has been the typical of attention since a major, government-led study found various other benefits - it shortened restoration time for hospitalized clients by five days typically, from 15 days to 10.
Within the US, a federal government guidelines panel and some top-rated medical groups have not endorsed two other therapies the meals and Drug Administration authorized for emergency use - Eli Lilly's experimental antibody drug and convalescent plasma, the blood of COVID-19 survivors. The teams say there isn't enough evidence to advise for or against them.
Doctors also remain uncertain about when so when not to utilize the only drugs recognized to improve survival for the sickest COVID-19 patients: dexamethasone or similar steroids. And stuff received murkier with Thursday's information that the anti-inflammatory medication tocilizumab may help. Just like the key WHO analysis on remdesivir, the preliminary benefits on tocilizumab possess not however been published or fully reviewed by independent scientists, leaving doctors unclear about what to do.
"It's an authentic quandary," said the University of Pittsburgh's Dr. Derek Angus, who's involved in a report testing several treatments. "We need to see the facts." Dr. Rochelle Walensky, infectious disease chief at Massachusetts Standard Hospital, agreed."It's very difficult to apply for medicine by news release," she said on a podcast Thursday with a medical journal editor. Before National Institutes of Health's guidelines endorse a treatment, "I'm actually reluctant ... to phone that standard of health care."
This week, the Institute for Clinical and Economic Review, a nonprofit group that analyzes drug prices, said remdesivir should be priced around $2,470 for hospitalized patients with moderate to severe disease because of the cost savings from fewer days of care. On the other hand, it's worth only $70 for clients hospitalized with milder disease, the group concluded.
In another development, the FDA on Thursday gave urgent authorization to usage of another anti-inflammatory drug, baricitinib, to be used with remdesivir. Adding baricitinib shaved an additional day off the common time to recovery for severely ill hospitalized clients in one review. Lilly sells baricitinib right now as Olumiant to treat arthritis rheumatoid, the less common sort of arthritis that occurs whenever a mistaken or overreacting disease fighting capability attacks joints, leading to inflammation. An overactive immune system also can result in serious challenges in coronavirus patients.